Optometrists can now, more than ever, address the issue of chronic dry eyes using advanced technology.
Eyecare Plus Chullora optometrist Dr Kerry Ho joined the OMEGA 19 this year hosted in Melbourne. The conference showcases a series of presentations which highlighted upcoming research and outbreaks in the field of optometry.
One of the points of focus was dry eye, a condition which has been shown to affect up to 50% of the population and is known to have significant impact on work productivity.
Here are Kerry’s highlights:
Despite the prevalence of it, Dry Eye Syndrome has been underdiagnosed and often undertreated. One of the reasons is because there are many complex factors which contribute to this condition, thus it is difficult to accurately diagnose the type of dry eye and in turn manage the causative factor.
Dry eyes can often be masked by other conditions or can be asymptomatic until it reaches an irreversible severe stage. Thus, patients will often ignore this condition, question the diagnosis, or the optometrist may just choose to leave it untreated.
Several talks at OMEGA 19 focused on the research of the Tear Film and Ocular Surface Society’s study called the TFOS DEWS II, which aimed to simplify the process of diagnosing and treating dry eyes.
The primary causative factor of dry eyes was hyperosmolality, which would trigger a cyclical series of events to worsen the state of the eye. The two primary types of dry eyes are aqueous deficient and lipid deficient dry eyes, although most patients will suffer from both forms.
The Latest Equipment and Technology
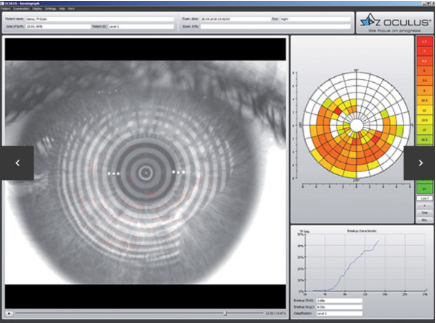
As part of the conference, two equipments have been manufactured to help practitioners, namely the Keratograph (Fig 1) and the Medmont Topographer (Fig 2).
Functionally, both these machines allow one to access several components of dry eyes. They measure the Tear Break Up Time (TBUT) which in turn measures the stability of the tear film. The Keratograph in particular allows one to determine the local spots on the eye which dry eye first occurs (Fig 3) and the time that sector broke up.
Figure 3
Both allow a fluorescein fit, which allows one to assess the TBUT and contact lens fit. Both also offer an examination of the meibography, which allows one to assess the integrity of the Meibomian glands which are responsible for the production of lipids in the tear film (Fig 4).
Figure 4
The Keratograph also allows one to measure the amount of tears produced by assessing the height of the tears against the lower eyelid.
Another strong function of the Keratograph is that it integrates all these findings along with the patient’s symptoms into a qualitative and quantitative analysis, which allows the patient to more easily understand the state of their dry eyes. More importantly, it will allow practitioners to demonstrate changes before and after treatment (Fig 5).
Figure 5
Overall, the OMEGA 19 conference has provided significant information, and the industry has offered practitioners equipment to more successfully diagnose and treat dry eyes. The Keratograph seems most promising with its ability to assess the components of dry eyes then integrate the results into a format which is more readily understood by the practitioner.
With all this information, optometrists should more directly address the ever-present issue of dry eye in the community.